Claim Denial Minimization – Unlock What You Need to Know
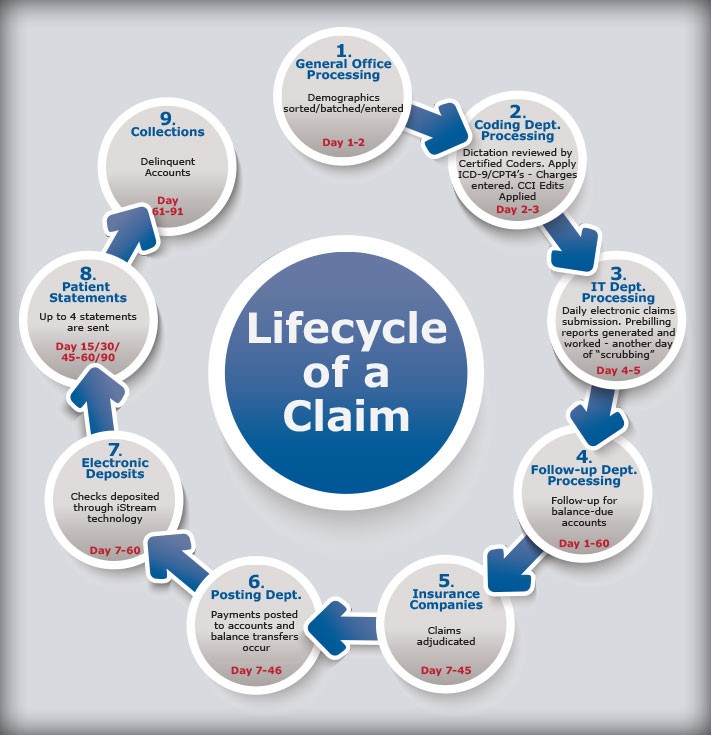
Claim denial Minimization, according to the Medical Group Management Association (MGMA), even the best-performing medical practices have denied 4 percent of their claims. MGMA estimates that up to 65 percent of denied claims are never re-submitted. It costs approximately $25 to re-submit a denied claim. To ensure that we receive payment for all claims submitted, it is crucial to thoroughly investigate any rejected claims, address and correct any errors promptly, and resubmit them within the 90-day timeframe. This process helps to maximize our reimbursement and ensures that we are not missing out on any potential revenue. Failure to do so may result in delayed or denied payment. Neglecting to do so may result in non-payment.
 Prevention
Prevention
Of course, the best way to minimize medical claim denial is to prevent them in the first place. Thus the medical billing professionals of ebix, Inc. make sure that all our medical claims are “clean.” To put it another way, a clean medical claim meets the requirements stated by insurance providers for payment on the first submission. A sterile medical claim begins at the first point of contact. Patient registration has been accurately completed and all primary, secondary, and tertiary insurance policies have been successfully confirmed.
Never Settle
As a medical practice, you should never settle for a first-time claim denial as a typical occurrence. Every rejection is worth fighting for, and taking proactive measures to prevent recurring claims denials is crucial. When a health insurance company denies a claim, it’s essential to take the necessary steps to appeal and reverse the decision. Not only can this help increase your revenue, but it will also ensure that your patients receive the proper care they need.
Don’t simply accept a denied claim and move on. Fight to overturn the decision and advocate for your patient’s well-being. By doing so, you’ll be positively impacting the healthcare industry. We investigate the reason for the rejection and minimize medical claim denials. Our team of expert claim resolvers at ebix ensures that your practice’s medical claims are processed efficiently and with utmost precision. And when necessary, we offer extensive practice education and training sessions.
What we do:
- Conduct accurate demographic and insurance registration of patients.
- Meet timely filing deadlines.
- Reconciliation of medical service provided to match the procedure code.
Contact us for a Complimentary Consultation.
Download Brochure ebix Minimize Claim Denials PDF.